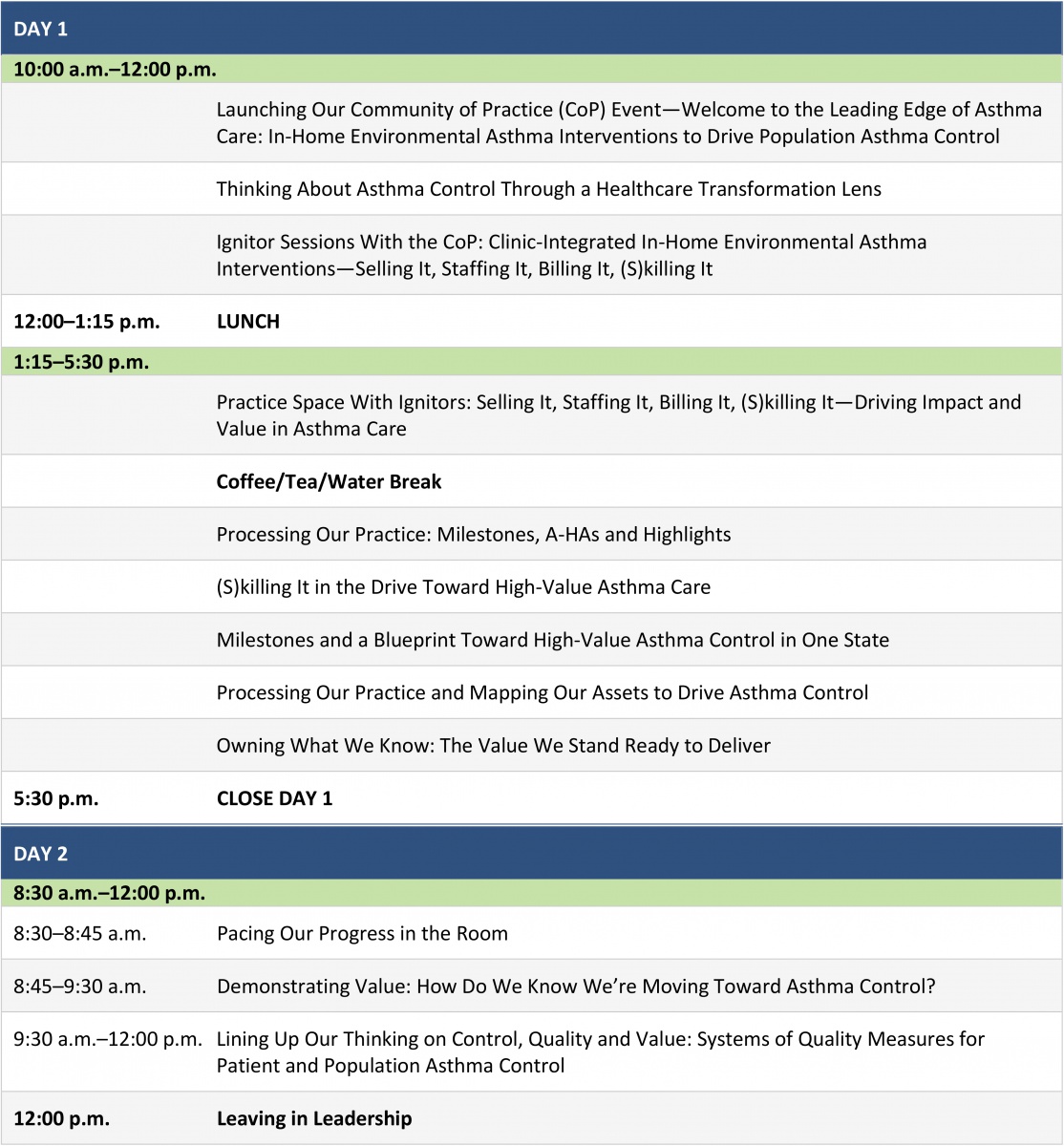
The meeting addressed a broad agenda, including—
- Making the leap from program level to health care–system level while championing in-home environmental asthma interventions as a key to population asthma control.
- Measuring progress in asthma care, quality measurement in asthma home-intervention practice and standards, and emerging measures to assess health and housing impacts from integrated clinic and community-based work.
- Discussing the concept of “value” in health care, an ongoing national dialogue that environmental health practitioners, community health workers and other “nontraditional” providers of health care can influence and to which they have much valuable experience and wisdom to offer.
The group considered potential measures and data that could be gathered across an integrated, high-quality asthma-care system, as well as the types of data that would demonstrate health outcomes achieved in real time, over time and at the population scale across a community. The participants explored how to assess the effects that in-home interventions for asthma care have on patient health and experience, as well as on patient and family quality of life. The group explored how to evaluate the impact of integrated clinic and community care models on provider experience, total costs of health care, and communities as a whole. Although the ideal mechanisms and instruments for measurement are not defined yet, there was widespread agreement that the field of asthma care would benefit from the development of national standard outcomes measures that improve on the medication-based measures predominant today. Participants engaged in a robust discussion about the potential strengths and drawbacks of a quality measure for patient asthma control and a request for federal and national action to advance exploration of asthma control as a potential quality measure that may drive improved practice and improved health for people with asthma.
EPA’s Community of Practice intends to continue exploring health care reimbursement developments related to expanded financing for in-home asthma care services, quality measures for asthma control and research to support their development, and discussions of value in asthma care related to clinical and community integrations of care. More information will be shared as it is available.